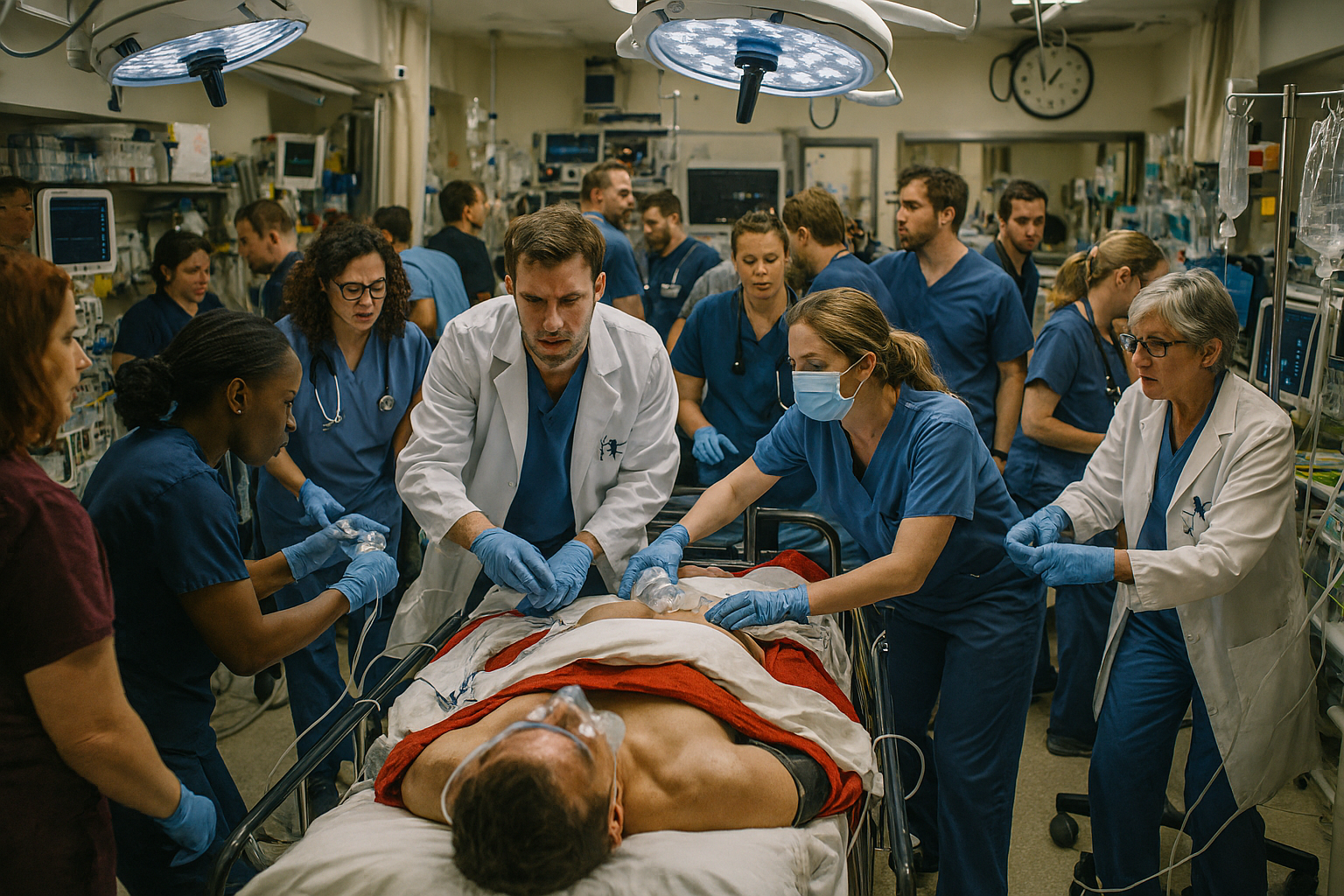
Common Pitfalls in Crowded Trauma Bays: An Examination of Controlled Chaos
Trauma activations are equal parts choreography and chaos—an adrenaline‑tempered ballet performed in a room the size of a studio apartment but somehow containing 20 humans, four IV poles, two ultrasound machines, and the universal belief that everyone is essential. Despite the high stakes and heroic efforts, overcrowding and unclear workflows can turn even the most seasoned trauma team into a well‑meaning herd of cats. Understanding the common pitfalls helps ensure that what feels like chaos doesn’t devolve into actual compromise of patient care.
Pitfall 1: Role Confusion—When Everyone’s Helping but No One’s Helping
One of the most persistent issues in crowded trauma bays is unclear or overlapping roles. Without explicit role assignment, clinicians gravitate toward tasks based on habit, comfort, or proximity—sometimes resulting in three people starting an IV while no one is managing the airway. Research highlights that failure to assign responsibilities leads to inconsistent communication, inefficient workflows, and ultimately poorer patient outcomes (Tien et al., 2025).
Similarly, early interviews with developing trauma programs show that staff often jump in without structure simply because trauma is exciting—and who wants to miss the action? (Guerrero, 2019).
Takeaway:
If everyone thinks they’re the team leader, no one is the team leader.
Pitfall 2: Crowding for Curiosity’s Sake
Trauma brings spectators—well‑meaning clinicians who want to help or learn. Unfortunately, good intentions can block access, disrupt sterile fields, and increase stress. Programs transitioning to trauma center status often report that early responses are hampered not by lack of resources but by “too many cooks in the kitchen” (Guerrero, 2019).
Efforts like floor markings and color‑coded lead aprons have demonstrably improved crowd control and workflow by clarifying exactly who should be standing where (Tien et al., 2025).
Takeaway:
The trauma bay is not a flash mob—if your position isn’t choreographed, you probably shouldn’t be in the dance.
Pitfall 3: Parallel Conversations and Communication Fog
Even the most organized trauma team can fall prey to competing conversations, incomplete callouts, and half‑closed loops—especially under duress. Multiple studies show that communication and interaction consistently rank as the weakest non‑technical skills during trauma activations (Bhangu et al., 2022).
Incomplete closed‑loop communication and multiple simultaneous conversations persist irrespective of case severity, which can lead to errors in medication administration, airway strategy, or diagnostic sequencing (Bhangu et al., 2022).
Takeaway:
If three people answer a question that no one actually heard, was communication ever really achieved?
Pitfall 4: Loss of Situational Awareness
Overcrowding amplifies noise, movement, and cognitive load—conditions that degrade situational awareness. Team performance literature repeatedly ties loss of shared mental models to delays in decision‑making and missed critical cues (Barach & Weinger, n.d.).
Teams that lack situational awareness behave more reactively than proactively, creating a clinical environment where interventions lag behind deterioration.
Takeaway:
A trauma bay without situational awareness is like driving through fog with your high beams on—you feel like you’re improving visibility, but you’re actually blinding everyone.
Pitfall 5: Lack of Identifiers—Who Are All These People?
In crowded trauma bays, distinguishing who is who—especially during shift changes—is surprisingly difficult. Innovations such as color‑coded caps, lead aprons, and role stickers significantly improve communication and reduce redundant movement by making team members recognizable at a glance (Andrews & Paulasir, 2024).
Takeaway:
If the trauma bay were a superhero movie, everyone deserves a costume—preferably one that labels their superpower.
Conclusion
Trauma resuscitation will never be calm, but it can absolutely be controlled. Implementing structured roles, crowd‑management tools, communication training, and visual identifiers transforms chaos into coordination. As trauma professionals, we owe our patients not only speed and skill but also systematic teamwork.
So here’s the challenge:
Whether you’re a trauma coordinator, charge nurse, resident, or leader—pick one improvement (role cards, pre‑briefs, visual markers, comms training) and champion it. Small, consistent changes compound into safer, smoother, smarter trauma bays.
References
Andrews, E., & Paulasir, S. (2024). The colored cap project [Poster Presentation]. Henry Ford Jackson Hospital Research Symposium. https://scholarlycommons.henryford.com/hfjhrs2024/11/
Barach, P., & Weinger, M. B. (n.d.). Trauma team performance. AIA Seattle. https://aiaseattle.org/wp-content/uploads/2015/01/ITTACS-Team-Performance.pdf
Bhangu, A., Notario, L., Pinto, R. L., Pannell, D., Thomas‑Boaz, W., Freedman, C., Tien, H., Nathens, A. B., & da Luz, L. (2022). Closed loop communication in the trauma bay: Identifying opportunities for team performance improvement through video review analysis. Canadian Journal of Emergency Medicine, 24(1), 415-422. https://doi.org/10.1007/s43678-022-00295-z
Guerrero, A. (2019). How we did it: Defining roles and preventing crowding in the trauma bay. Trauma System News. https://trauma-news.com/2019/08/how-we-did-it-defining-roles-and-preventing-crowding-in-the-trauma-bay/
Tien, L., Sturdevant, M., Javangula, M., Ange, B., McKenzie, J., Medeiros, R., Adam, B., Abuzeid, A., Switzer, E., Lee, A., & Simmerman Mabes, E. (2025). Remodeling the trauma bay to improve communication and patient care: A novel approach to trauma resuscitations. Trauma Surgery & Acute Care Open, 10(2). https://tsaco.bmj.com/content/tsaco/10/2/e001689.full.pdf