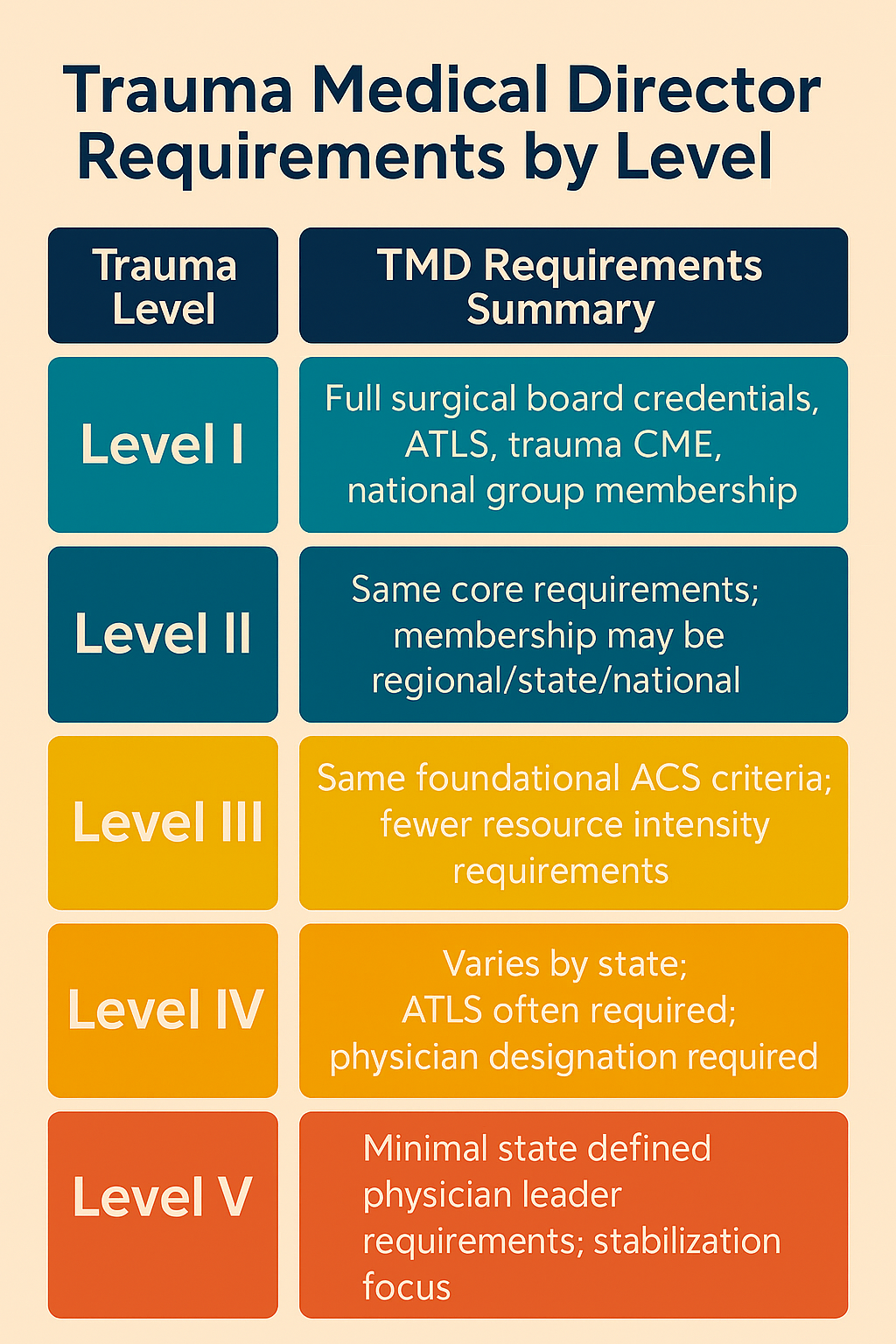
Trauma Medical Director Essentials: How to Meet ACS Requirement Without Flatlining Your Sanity
Across trauma centers nationwide—whether Level I titans or Level V frontier outposts—the Trauma Medical Director (TMD) is the anchor of trauma leadership. Part clinician, part process improvement guru, part diplomat, this role blends medical expertise with operational stewardship.
________________________________________
1. Levels I–III: ACS Defined Trauma Medical Director Requirements
For all ACS verified trauma centers—Levels I, II, and III—the TMD must meet uniform national standards established by the American College of Surgeons Resources for Optimal Care of the Injured Patient (American College of Surgeons, 2025).
Board Certification Requirements
The TMD must:
Hold current board certification or be board eligible in
General surgery or
Pediatric surgery
Accepted boards include:
American Board of Medical Specialties (ABMS)
American Osteopathic Association (AOA)
Royal College of Physicians and Surgeons of Canada (RCPS C)
(American College of Surgeons, 2025)
Program Leadership
Must serve as the director of one trauma program only.
Must be credentialed to provide trauma care (American College of Surgeons, 2025).
Required Trainings & Certifications
Advanced Trauma Life Support (ATLS®) — must be current.
Must participate on the trauma call panel.
Continuing Education Requirements
The TMD must provide evidence of 36 hours of trauma related CME during each verification cycle.
Pediatric TMDs: At least 9 of the 36 hours must be pediatric specific.
Up to 30 hours of board certification/recertification CME may be counted once per cycle.
For initial verifications: Minimum 12 hours of trauma CME (American College of Surgeons, 2025).
Trauma Organization Membership
Depending on verification level:
Level I: Must hold active membership in at least one national trauma organization and attend a meeting once per cycle.
Level II–III: Must hold state, regional, or national trauma organization membership and attend a meeting once per cycle (American College of Surgeons, 2025).
Note: Membership in an ACS State Committee on Trauma (COT) does not count as national membership.
Special Requirements for Pediatric TMDs Who Are Not Pediatric Surgeons
If a general surgeon serves as pediatric TMD, the center must also ensure:
TMD holds current PALS certification.
A written affiliation agreement exists with a pediatric TMD at an ACS verified Level I pediatric trauma center.
Agreement must include:
Assistance with PI, guideline development, and complex case discussions
Attendance at ≥50% of multidisciplinary trauma PI meetings
Participation in the ACS VRC site visit
(American College of Surgeons, 2025)
Measures of Compliance for Levels I–III
Site reviewers will look for:
Board certification/eligibility documentation
Role descriptions
Credentialing letter
ATLS certificate
Call schedule
CME certificates
Trauma organization membership
If pediatric TMD exception applies:
PALS certificate
Affiliation agreement
Attendance records
________________________________________
2. Levels IV and V: State Determined Requirements
(Where Details Vary Widely)
Unlike Levels I–III, the ACS does not verify Level IV or V centers.
This means each state defines its own TMD requirements, resulting in notable variability.
Examples from State Regulations:
Colorado
Colorado requires that the TMD simply be:
A physician designated by the facility
No surgical board certification or specialty is mandated (Colorado Department of Public Health & Environment, 2025).
Texas
Texas requires Level IV TMDs to:
Maintain ATLS or equivalent
Hold clinical oversight authority in:
Trauma PI
Protocol development
Credentialing
Direct trauma care
(Texas Department of State Health Services, n.d.)
Minnesota
Minnesota requires Level IV TMDs to:
Meet the same trauma training requirements as emergency physicians
Participate in PI and tertiary case review
(Minnesota Department of Health, 2023)
Conclusion: Requirements for Level IV–V TMDs depend entirely on state trauma systems—not ACS national standards.
________________________________________
________________________________________
3. Why the Difference?
Levels IV–V Serve a Different System Role
Because Levels IV and V focus on:
Immediate assessment
Stabilization
Transfer coordination
States design their criteria around:
Rural workforce availability
Regional trauma referral patterns
Local infrastructure
This flexibility keeps trauma systems functional across diverse geographies.
References
American College of Surgeons. (2025). Resources for optimal care of the injured patient (2022 standards; July 2025 rev.). https://www.facs.org/quality-programs/trauma/quality/verification-review-and-consultation-program/standards/
Colorado Department of Public Health & Environment. (2025). Trauma facility designation criteria – Level IV and V. Colorado Code of Regulations. https://slvretac.org/wp-content/uploads/2024/02/6-CCR-1015-4-Chapter-3_Designation-of-Trauma-Facilities.pdf
Minnesota Department of Health. (2023). Level 4 trauma hospital designation criteria. https://www.health.state.mn.us/facilities/traumasystem/documents/criteria_level4.pdf
Texas Department of State Health Services. (n.d.). Basic (Level IV) trauma facility criteria checklist. https://www.dshs.texas.gov/sites/default/files/emstraumasystems/critIVtable.pdf